
How Does the Lymphatic System Work—and Why Should You Care?
April 22, 2026
When to Recognize It’s Time for Professional Help During Recovery
April 22, 2026A Holistic Path to Recovery
Integrated post‑surgical care that couples physical therapies with emotional support is essential for women recovering from cosmetic or reconstructive procedures. Research shows that stress hormones such as cortisol slow wound healing, while compassionate communication and counseling lower anxiety and boost immune function. Lymphatic drainage massage, a core service at Pink & Fancy, reduces swelling, improves circulation, and creates a calming sensation that further reduces cortisol. The boutique’s team, led by an OR nurse with 25 years of experience, blends evidence‑based techniques—manual lymphatic therapy, wood therapy, gentle exercise—with personalized mindfulness, guided imagery, and open dialogue. This seamless integration empowers patients to feel heard, adhere to rehab plans, and experience faster tissue repair and greater overall wellness. Patients gain significantly lasting confidence each day.
Post‑Surgery Depression and Anxiety

Post‑surgery depression and anxiety are common, situational responses that can arise from pain, swelling, altered appearance, and the stress of recovery. Pre‑existing mental‑health conditions, the type of anesthesia used, and a lack of realistic expectations heighten the risk, while strong social support, early screening, and clear communication with the care team protect resilience. Common emotional responses after surgery include sadness, irritability, fear of complications, and a sense of loss of control. Risk factors such as prior depression, high postoperative pain, and financial worries interact with protective factors like supportive family, compassionate counseling, and personalized education. Physical therapies that ease emotional distress include gentle movement (light stretching or short walks) that releases endorphins, and manual lymphatic drainage massage, which reduces swelling, improves circulation, and lowers cortisol levels. When combined with mindfulness, guided imagery, and regular check‑ins with a therapist, these interventions create a holistic recovery plan that addresses both mind and body, helping women regain confidence and accelerate healing.
Healing Therapy Techniques for Women Recovering from Surgery

Healing therapy for women after surgery combines gentle, low‑pressure techniques that move lymph and reduce swelling while supporting tissue repair. Manual lymphatic drainage—performed by a certified therapist or taught as a self‑massage routine—uses light, rhythmic strokes to guide excess fluid toward healthy lymph nodes for removal. This method lowers cortisol, eases anxiety, and accelerates edema reduction, which is especially valuable after cosmetic or reconstructive procedures.
Complementary modalities such as wood therapy, soft‑tissue mobilization, and guided stretching further improve circulation and restore range of motion without stressing healing incisions. Wood therapy stimulates micro‑circulation, while soft‑tissue mobilization releases muscular tension that can impede lymph flow. Carefully prescribed stretching activates the parasympathetic nervous system promoting joint mobility and confidence.
Mind‑body practices—including yoga, deep‑breathing, and meditation—lower stress hormones, enhance blood flow, and reduce perceived pain. These interventions help patients maintain a positive outlook, improve sleep quality, and support immune function, creating a holistic environment that speeds tissue repair and promotes overall well‑being.
Post‑Operative Trauma Symptoms

Surgical trauma can leave a psychological imprint that mirrors the physical injury. Patients often experience intrusive memories of the operating room, vivid flashbacks, and a relentless mental replay of the procedure, which can trigger heightened startle responses and hyper‑vigilance toward pain or complications. These mental stressings frequently disrupt sleep, leading to difficulty falling asleep, frequent awakenings, or nightmares that replay surgical details. The resulting fatigue interferes with daily functioning, diminishing concentration, motivation, and the ability to engage in prescribed rehabilitation activities. Early interventions are essential: coordinated care that blends compassionate communication, counseling, and mind‑body techniques such as guided imagery, meditation, and deep‑breathing can reduce cortisol, improve mood, and promote better sleep. Integrating Lymphatic drainage massage not only eases physical swelling but also provides a soothing, tactile experience that lowers anxiety. By recognizing trauma symptoms promptly and offering personalized, multidisciplinary support, clinicians help women recover both mentally and physically, fostering confidence, adherence to therapy, and a smoother overall healing journey.
The Mind‑Body Connection in Recovery

The mind‑body connection means that our thoughts, emotions, and stress levels directly affect how quickly tissue repairs and how much inflammation we experience after surgery. A calm, positive mindset can lower cortisol, improve circulation, and support the lymphatic system’s ability to clear fluid and toxins.
How thoughts and emotions affect tissue repair – Psychological stress raises cortisol which suppresses immune function and slows collagen synthesis, while supportive emotions boost immune activity and reduce pain perception.
Cortisol reduction through relaxation – Practices such as guided imagery, meditation and gentle breath‑work activate the parasympathetic nervous system, decreasing cortisol by up to 12 % and allowing faster wound healing and less swelling.
Practical breath‑work and gratitude practices – Simple diaphragmatic breathing (4‑7‑8 pattern), short gratitude journaling, and visualization of healing tissues can be done twice daily. Combined with lymphatic drainage massage or light walking, these techniques enhance lymph flow, lower anxiety, and accelerate functional recovery.
By nurturing both mental wellbeing and physical care, women recovering from cosmetic or reconstructive surgery can reduce inflammation, improve swelling, and thrive in their post‑operative journey.
Nutrition, Supplements, and Fluid Strategies for Optimal Healing
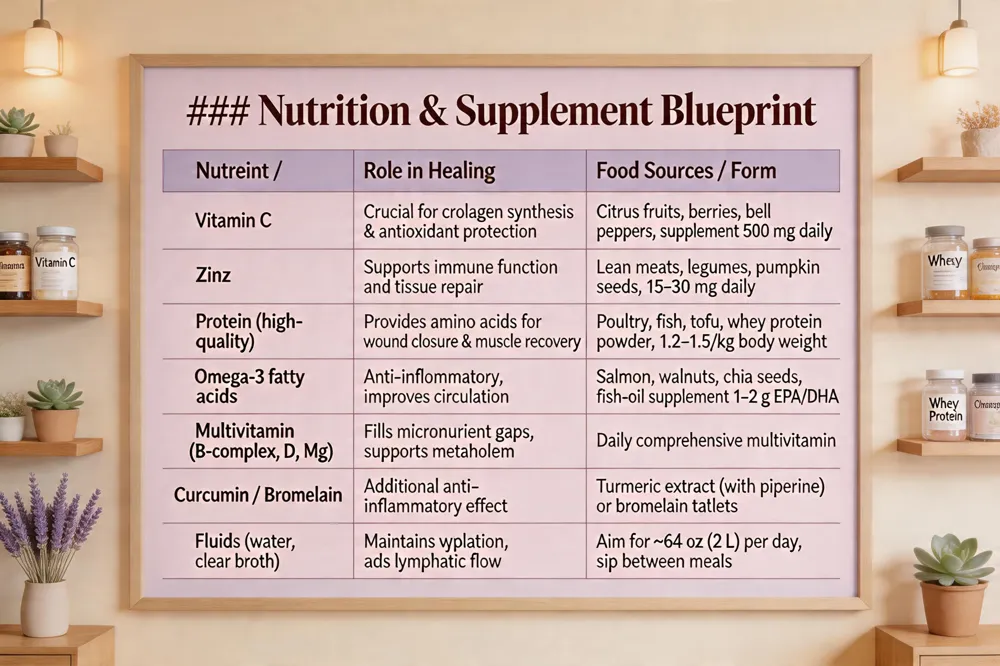
A well‑planned post‑surgical diet is a cornerstone of rapid tissue repair, reduced swelling, and overall well‑being—especially for women recovering from cosmetic or reconstructive procedures. The body’s healing engine needs adequate calories, high‑quality protein, vitamins, minerals, and fluid to support immune function, collagen synthesis, and lymphatic drainage. Below are evidence‑based recommendations that integrate key nutrients, anti‑inflammatory foods, sensible supplementation, and a step‑by‑step liquid‑to‑solid progression.
Key nutrients that speed tissue repair
Collagen formation hinges on vitamin C, zinc, and sufficient protein. Lean sources—poultry, fish, tofu, legumes, or a high‑quality protein powder—supply the amino acids required for wound closure and muscle recovery. Omega‑3 fatty acids (fish oil or algae) temper post‑operative inflammation, while a broad‑spectrum multivitamin covering B‑complex, vitamin D, and magnesium fills any nutritional gaps that could slow healing.
Anti‑inflammatory foods to reduce swelling
Leafy greens (spinach, kale), bright berries, and citrus fruits deliver antioxidants and vitamin C that curb edema. Omega‑3‑rich foods such as salmon, walnuts, and chia seeds further dampen inflammation and improve circulation. Incorporating bone broth or lean poultry provides protein without excess fat, supporting both tissue repair and a calm inflammatory response.
What to avoid and why
High‑sodium processed foods (deli meats, canned soups, salty snacks) trap fluid and exacerbate swelling. Sugary treats and refined carbs spike inflammation and impair immune function. Alcohol and excessive caffeine dehydrate the body and interfere with natural repair processes. Fried, greasy meals and heavy red‑meat portions are harder to digest and can increase postoperative inflammation. Opt instead for low‑sodium, whole‑food choices.
Liquid diet progression after surgery
Start with clear liquids—warm broth, diluted fruit juice, caffeine‑free herbal tea to stay hydrated without straining digestion. Advance to full‑liquid options like strained creamy soups, low‑fat milk, gelatin desserts, and protein‑enriched smoothies. Once tolerated, introduce pureed foods (blended cottage cheese, pureed vegetables) to boost protein and vitamin intake. Aim for about 64 oz (2 L) of fluid daily, sipping between meals.
Supplement recommendations for faster recovery
Vitamin C and zinc are essential for collagen production and immune support, accelerating wound closure and reducing infection risk. Adequate protein, whether from whole foods or a quality powder, supplies the building blocks for tissue repair. Omega‑3 supplements curb swelling and bruising. A comprehensive multivitamin ensures coverage of B‑complex, vitamin D, and magnesium. Anti‑inflammatory botanicals such as curcumin (turmeric) or bromelain can further calm the inflammatory response.
By following this balanced, anti‑inflammatory nutrition plan and incorporating targeted supplements, women can support their lymphatic system, reduce edema, and promote a smoother, faster recovery.
Advanced Physical Therapy, Energy Practices, and Trauma‑Focused Care

Emerging physical‑therapy modalities for women after surgery include instrument‑assisted soft‑tissue mobilization (IASTM), low‑frequency electrical stimulation, and proprioceptive neuromuscular facilitation (PNF) that are customized to protect incisions while restoring range of motion and lymph flow. Complementary spiritual and energy‑healing practices such as guided meditation, Reiki, intention‑focused breathing, and gentle movement meditation calm the autonomic nervous system, lower cortisol, and promote fluid drainage, which can reduce postoperative swelling and anxiety. A brief daily body‑scan or grounding meditation further supports the lymphatic system and eases inflammation. Post‑surgical traumatic stress syndrome (PTSS) can arise after a frightening operative experience and presents with intrusive memories, avoidance, sleep disruption, and heightened arousal; roughly 20 % of patients develop clinically significant symptoms. Early screening and a multidisciplinary plan that blends trauma‑focused psychotherapy (CBT, EMDR) with gentle lymphatic massage improves outcomes. The 4 C’s of wound healing—Cellular Response, Coagulation, Contamination, and Closure—guide clinicians in managing tissue repair. Most women’s postoperative depression resolves within 2–6 weeks, though complications can prolong it.
Putting It All Together for Thriving Recovery
Recovery after cosmetic surgery thrives when body and mind work together. Scientific studies show that reduced cortisol, better immune function, and faster tissue repair follow relaxation, mindfulness, and supportive counseling. For women, a practical plan includes: 1) Follow a protein‑rich, vitamin‑C diet and stay hydrated; 2) Begin gentle ambulation and lymphatic drainage massage within 24‑48 hours to lower swelling and boost circulation; 3) Practice deep‑breathing or guided meditation for 10‑15 minutes to calm stress hormones; 4) Keep a recovery journal and schedule regular check‑ins with a therapist or loved one; 5) Use compression garments and posture cues to protect incisions. Pink & Fancy tailors each step to goals, offering certified lymphatic therapists, personalized nutrition guides, and counseling that together create an empowering healing journey.




